Heller School researchers focus on a visionary approach to improving eyesight
They assess the clinical and economic benefits of the scleral lens
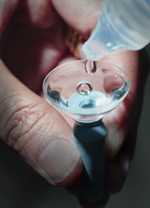
Boston Ocular Surface Prosthesis
Joseph Balboni loves sports. An avid tennis player and golfer, as well as baseball fan, the 46-year-old insurance agent became increasingly frustrated over time as his eyesight dimmed due to keratoconus, a degenerative eye disorder. Unable to return the tennis ball or see the pitch at Red Sox games, he faced the prospect of a corneal transplant to restore his vision and eye comfort.
Then three years ago, Balboni discovered an alternative treatment. He received a gas permeable scleral lens (covering the white of the eye) known as the Boston Ocular Surface Prosthesis (BOS-P) from the Boston Foundation for Sight in Needham, Mass. “The scleral lens changed my life,” said Balboni. “I am very fortunate because the corneal transplant is an expensive operation with no guarantee of lasting results.” Balboni’s insurance company paid for the lion’s share of the roughly $8,000 for treatment and fitting of the lens, even though insurance coverage of the lens is not routine.
Today, in the December issue of the American Journal of Ophthalmology Brandeis University researchers published a paper appraising the economic benefits of the BOS-P, a highly precise scleral lens used to treat severe cornea or ocular surface disease. A companion paper on the clinical benefits has been published online and will appear in the journal’s January issue.
The lens is custom fitted to the eye, vaulting the cornea while submerging the entire corneal surface in a pool of oxygenated artificial tears. Designed to improve vision, reduce eye pain, mitigate light sensitivity, and heal and protect the ocular surface, the lens is used in patients with eye diseases including keratoconus, Stevens-Johnson syndrome, dry eye syndrome, and chronic graft vs. host disease. The BOS-P is also useful in patients whose visual acuity is compromised after many types of eye surgery.
The studies were conducted by a team of researchers at the Heller School that included William B. Stason, MD, a senior scientist, Donald Shepard, PhD, a professor and researcher, Moaven Razavi, MS, a research associate and PhD candidate, and Deborah S, Jacobs, MD, an ophthalmologist at the Boston Foundation for Sight and Harvard Medical School.
The clinical study assessed visual acuity and visual functioning in 69 patients before and after being fitted with a BOS-P. Using a scale from the National Eye Institute, the researchers reported highly significant improvements in visual functioning scores (from 57.0 to 77.8 on a scale of 0 to 100). Gains in visual acuity were also highly significant.
The economic analysis was then undertaken to assess the cost-effectiveness of the scleral lens for each patient fitted, as well as the economic value of resulting improvements in visual function. The researchers based the economic benefits on improvements in visual functioning and converted these to quality-adjusted-life-years (QALYs), a standardized measurement of health. The average cost-effectiveness of the prosthesis was $24,900 per QALY (a favorable value) and the average benefit-cost ratio was 4 to 1, and even higher, 5.6 to 1, in patients with especially severe eye disease.
The research team commented: “We were pleasantly surprised by the outcomes of our studies, because the scleral lens is an expensive device, but it turned out to be both cost-effective and offer a significant improvement in quality of life.”
The studies amplify what Joseph Balboni experienced as soon as he started wearing the BOS-P scleral lens: there is nothing like clear, pain-free vision to change your outlook on life.





