Medical Tourism and Public Health Care in Turkey
Nihal Kayali
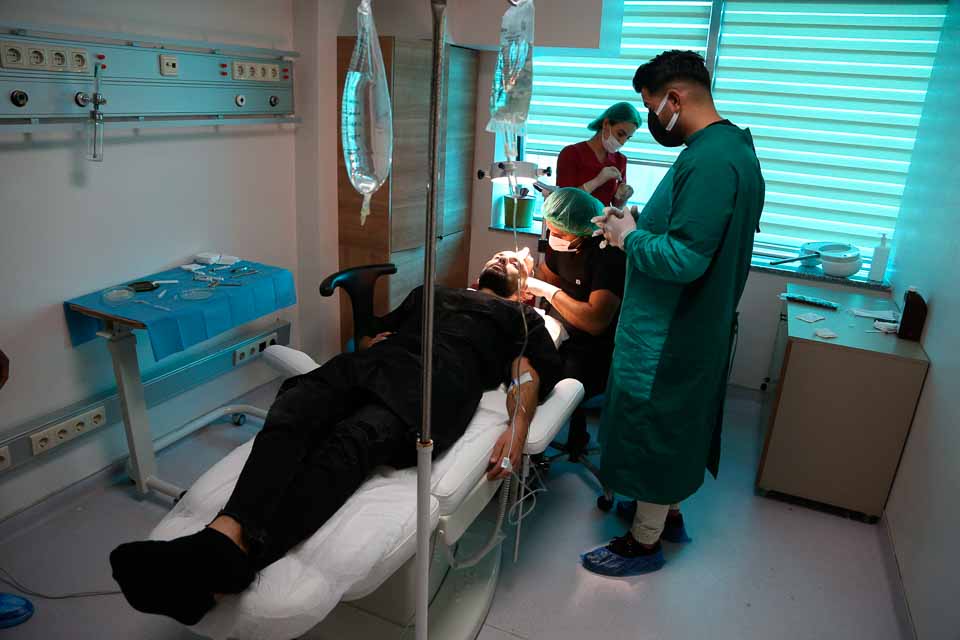
Hair transplant surgery at Bella Hair clinic in Istanbul, Turkey on September 19, 2021. Photo by Jerome Domine/Abaca/Sipa USA
Middle East Brief No. 168 | April 2026
At the height of the Covid-19 pandemic, public spaces across Turkey emptied out under strict government curfews that stretched from Friday evenings to the early hours of Monday mornings. Yet those who ventured to Istanbul’s tourist districts could encounter a curious exception: Foreign men with bandaged heads recovering from hair transplant surgeries remained conspicuously present on the city’s otherwise sleepy streets.[1] Although residents were confined indoors, the Turkish government had exempted foreigners from lockdown restrictions and had continued to court medical tourists. As early as May 2020, Turkey had reopened its borders to accept patients from thirty-one countries.[2]
The swift reopening of Turkey’s hospitals to international patients during the pandemic—even as domestic patients were advised to forgo nonurgent care—laid bare how central medical tourism had become to the government’s health care agenda. This same government, under the leadership of Recep Tayyıp Erdoğan and the Justice and Development Party (Adalet ve Kalkınma Partisi — AKP), had once prioritized health care reforms aimed at universalizing coverage for Turkish citizens. How did foreign patients come to occupy such an important place in Turkey’s health care system, and what has this shift meant for health care access at home?
This Brief examines the rise of medical tourism in Turkey and its implications for the country’s universal health care system. It argues that the state’s promotion of the medical tourism sector has contributed to widening inequalities in access to care for citizens. By incentivizing providers to capture foreign currency revenues from international patients, medical tourism has shifted institutional priorities away from domestic need. Technological investment, provider capacity, and labor have instead been channeled toward facilities that rely on revenue generation for their survival. Rather than benefiting from state support for this growing sector, citizens remain mired in an increasingly strained public health care system as providers train their gaze outward to international markets.
The Health Transformation Program and the Rise of Private Health Care
Turkey has catapulted itself into the popular imagination as the “hair transplant capital of the world”—a reputation reinforced through social media promotion, late-night comedy jabs, and a steady stream of “Turkish Hairlines” memes.[3] Cosmetic dental care, too, has become a globally recognized hallmark of the industry’s boom, as tourists flock to Turkey for full sets of “Hollywood Smile” veneers. Yet medical tourism in Turkey extends well beyond the cosmetic to a wide range of elective and even life-saving treatments, from cancer treatment to preventative imaging to heart surgery. Whether in Istanbul’s high-end hospitals or at its proliferating med-spas, medical professionals—doctors, nurses, technicians, and even aestheticians—increasingly administer care to visitors from abroad. Paradoxically, the restructuring of Turkey’s health care system to universalize access at home has facilitated this commercial turn.
Turkey’s pivot to medical tourism must be considered alongside the contemporaneous wave of privatization and market reform that has reshaped its health care system over the past two decades. In 2003, the Turkish government launched the Health Transformation Program (HTP), a sweeping health care reform initiated after the country’s severe economic crisis in 2001 and shaped by policies promoted by the International Monetary Fund and the World Bank. The HTP unified Turkey’s health system under the country’s General Health Insurance (Sosyal Güvenlik Kurumu — SGK), extending coverage to nearly all citizens.[4] Yet the HTP’s universalist insurance scheme was intertwined with institutional incentives linking coverage expansion to private-sector growth:[5] The SGK, for example, was restructured as a purchaser of services from both public and private hospitals. Private-care delivery, in this formulation, would augment public services and improve access for all. Yet as private providers became structurally dependent on revenue maximization, the boundaries between supplementing and supplanting public provision of health care services would grow less distinct.
The HTP health care reforms in fact led to a marked expansion of private hospitals. With the newly available windfall of SGK reimbursements, private hospitals became a profitable venture, and public money began to flow into hospital coffers. Ministry of Health reforms further encouraged investment in private hospitals by easing licensing rules. Providers were also permitted to charge patients co-payments up to twice the public insurance rates for standard treatments, and up to three times as much for “exceptional” treatments. By 2023, the number of private hospitals had exploded from 271 to 565, becoming key fixtures in health care provision across all of Turkey’s provinces.[6]
The pivot toward international patients emerged from the incentive structure built into the HTP reforms. As domestic SGK reimbursement rates were capped, providers increasingly sought revenue streams beyond the universal insurance framework. Foreign patients, who would pay full price for services, presented an attractive market for hospitals. Many newly minted private facilities born out of the favorable environment after the HTP reforms thus pivoted in that direction.[7]
Even public hospitals eventually became a venue for privatization under the HTP reforms. Since 2015, the government has backed the construction of public-private partnership “City Hospitals” (Şehir Hastaneleri), which are large-scale facilities financed by private consortia and leased to the Turkish government. While City Hospitals function like public hospitals, structurally they have shifted investment and profit to the private sector. The public sector, meanwhile, has assumed long-term risk with the specter of repayment obligations in foreign currency.[8] These gigantic hospitals have been promoted by the Ministry of Health as essential infrastructure to both serve Turkish citizens and attract medical tourists.[9]
The rapid expansion of hospitals in Turkey has become a new domain of political patronage, as ownership and construction of health care facilities became increasingly entangled with ruling party networks. Several private hospital groups with close ties to figures in AKP circles emerged after the HTP reforms, reflecting the muddying boundaries between public authority and private enterprise in Turkey during this period. The Medipol hospital group, for example, was founded by Fahrettin Koca, who would later become the Minister of Health under Erdoğan in 2018. Koca oversaw regulatory changes that expanded opportunities for private hospitals.[10] The opposition Republican People’s Party (Cumhuriyet Halk Partisi – CHP) has criticized state initiatives through which private hospital groups—notably those with multiple links to AKP figures—have received public financial support for medical tourism.[11]
It was not just the development of a revenue-generating hospital sector under the HTP that incentivized the provider pivot toward foreign patients. The Ministry of Health also restructured non-hospital services, establishing a clearer regulatory framework for private outpatient clinics and centers (poliklinikler and tıp merkezleri).[12] An expanding ecosystem of these smaller and more agile facilities absorbed ambulatory and elective care that proved particularly profitable. This expansion coincided with a sharp increase in health care capacity. Between 2002 and 2012, the health workforce grew by 56 percent, from about 295,000 to 460,000, while outpatient physician visits per capita nearly tripled.[13] The post-HTP increase in personnel and clinical space alongside broader marketization trends encouraged providers to extend treatment beyond traditional medicine and into aesthetic and elective care to tap higher-margin markets.[14]
The cosmetic health care sector is vast and loosely regulated. In 2016, an estimated six out of ten hair transplant clinics operated illegally.[15] These clinics would often employ technicians or nurses to perform procedures legally required to be performed by physicians, who sometimes merely lent their names for licensing purposes. Despite this informality—and indeed because of the proliferation of a lower-cost unregulated market—the state has benefited indirectly. Nevertheless, the explosion of the hair transplant industry has received such extensive global attention that in 2023, the Ministry of Health passed a Regulation on Hair Transplant Units to assert greater control over the burgeoning yet underregulated industry.[16]
Regulatory concerns have not diminished patient flows, however. The Turkish Health Tourism Association estimates that approximately one million people traveled to Turkey for hair transplants in 2022 and spent about $2 billion—roughly half of total health tourism expenditures in the country that year. Cosmetic dental care and plastic surgery, for their part, attracted estimated foreign patient expenditures of $500 million and $400 million, respectively.[17] Seizing on this profit potential, the Turkish government has thrown its policy weight behind the export of health care, with the goal of earning $20 billion in annual revenues from medical tourism by 2028.[18]
How Health Care Became an Export
Medical tourism existed in Turkey prior to the introduction of the HTP, but only as an ad hoc phenomenon. As the industry expanded, the Ministry of Health gradually assumed a larger steering role and made medical tourism a health care priority. This introduced an uneasy tension within the country’s health care system, as the same administration governing health care as a public good began to simultaneously operate according to export-oriented goals of growth and competitiveness. This contradiction has ushered in new forms of health care inequality within Turkey’s system, as care has been prioritized in high-revenue domains.
Turkey entered the medical tourism market later than both established destinations like Thailand and India and middle-income competitors like Mexico and Malaysia. Yet the country’s HTP-driven private sector expansion and Turkey’s strategic geographic position at the nexus of Europe, Central Asia, the Middle East, and Africa allowed it to grow rapidly. While initial recruitment focused on the nearby Balkans, it expanded to patients from the Middle East and post-Soviet states seeking advanced treatments. Europeans also began arriving at Turkey’s private hospitals in search of affordable and efficient care that their oversubscribed public systems struggled to provide. As these cross-border patient flows intensified, they went from being a marginal presence in Turkey’s health care system to an integral component of providers’ growth strategies, introducing new axes of differentiation among patients according to geography, mobility, and purchasing power.
Gradually, medical tourism went from being a marginal concern of the Ministry of Tourism to an object of interest within the Ministry of Health’s strategic planning. By the early 2010s, the state had adopted an increasingly proactive role in coordinating medical tourism—what Volkan Yılmaz and Püren Aktaş describe as “state entrepreneurialism.”[19] Yet this orientation also recalibrated the Ministry’s internal priorities, as export promotion became intertwined with the administration of universal care. This marked an important inflection point, as the Ministry of Health increasingly governed with two constituencies in mind: domestic citizens, entitled to universal coverage, and foreign patients, seen as sources of export revenue. Global branding efforts coordinated by the Ministry of Trade and the Turkish Exporters Assembly now beckon the world to come “Heal in Türkiye.”[20]
This export-oriented transformation of health care was mirrored within the Ministry of Health with the creation of Uluslararası Sağlık Hizmetleri Anonim Şirketi (USHAŞ), a state-owned company. Established in 2019, USHAŞ was tasked with managing and regulating Turkey’s medical tourism market while promoting Turkish health care institutions and professionals abroad. In 2022, this export-oriented approach was applied to domestic providers with the launch of HealthTürkiye, a digital platform managed by the Ministry of Health that providers could opt into for coordination or promotional purposes. By April 2025, a revised regulation mandated that all certified hospitals and brokers involved in medical tourism integrate into the platform in order to better regulate the sector.[21]
Some hospital administrators I spoke with interpreted the most recent reforms less as an affirmation of the government’s commitment to patient protection and more as an effort to redirect financial flows through a commercial platform. The Turkish Medical Association (Türk Tabipler Birliği — TTB) has in fact sued the Ministry of Health over its 2025 regulation, citing multiple legal concerns around provider autonomy, patient data privacy, price-setting, the legitimization of commission-based patient brokerage, and the manipulation of insurance markets.[22] In February 2026, this conflict erupted into health worker protests. Doctors and dentists explicitly rejected new Ministry of Health regulations requiring physicians treating foreign patients to register with USHAŞ and pay a 120,000 TL (about $2,700) authorization fee, arguing that the rule tied medical practice to a commercial license, thereby limiting physicians’ autonomy.[23] These professional objections and mobilizations point to the consolidation of an entire ecosystem of commercial actors and transactions under the umbrella of the Ministry of Health—a move that doctors see as institutionally prioritizing profits at the expense of citizens’ care.
By delegating the organization and promotion of health care to a state-owned company unencumbered by the constraints of public health care administration, the Ministry of Health has recast international health care as an explicitly market-oriented activity. This strategy introduces a fundamental institutional misalignment: The same ministry tasked with guaranteeing universal entitlement now operates within a framework that rewards revenue generation and international competitiveness. These dual incentives have gradually reshaped how resources, personnel, and regulatory attention are deployed.
Medical Tourism and Access to Care at Home
While medical tourism has boosted Turkey’s economy and international image, its expansion has affected citizens’ access to health care in uneven ways. These effects include transformations in hospital service priorities as well as shifts in the distribution of health care workers, as brain drain and market demands reshuffle the health care labor force. As provider priorities shift, local patients face the prospect of fewer doctors and longer wait times in neglected public hospitals.
The broader trend of privatization set in motion by the HTP has been amplified by hospitals’ turn toward the international patient market. Many private hospitals have developed expansive international patient offices, with multilingual staff and translators, while larger conglomerates have opened brick-and-mortar recruitment offices abroad. Acıbadem, Turkey’s largest private hospital group, has gone even further, establishing full-fledged hospitals in Serbia, North Macedonia, Bulgaria, and the Netherlands. Though high-quality services at private hospitals like Acıbadem are available to citizens at home as well, it is only the wealthy professional classes who can complement high costs with private insurance or out-of-pocket payments.
Meanwhile, as of 2025, eighteen public-private partnership City Hospitals had been built to serve both SGK-insured patients and, at least on paper, the burgeoning demands of medical tourists. For many Turks, these facilities have come to symbolize lavish investment in endless construction projects rather than structural improvement of the public system. Undeterred by concerns about the marketization of public health care providers, the Ministry of Health has recently launched USHAŞ Plus, a pilot program integrating twenty-nine public hospitals into medical tourism.[24] In the meantime, Turkish citizens remain nominally covered by universal insurance, but the public health system suffers as private hospitals distort the allocation of health care capacity. More than one-third of hospitals are now private, yet only 6.3 percent of all doctors’ visits occur there, leaving public facilities to shoulder the overwhelming majority of care.[25]
As public funding shifts toward profit-oriented models and private capacity grows, recent data suggest that health outcomes are stalling at best and deteriorating at worst. Between 2023 and 2025, the number of deaths avoidable with timely health care intervention, known as treatable mortality, increased from 107 to 119 per 100,000 people. Preventable mortality, or deaths that could be avoided through primary preventative care, rose even more, from 126 to 168 per 100,000 people. Moreover, declines in infant and child mortality have stalled in recent years, remaining well above numbers for other developed countries.
Turkish patients perceive these shortcomings: Their satisfaction levels compare unfavorably with those of patients in other developed countries in the Organisation for Economic Co-operation and Development (OECD). In 2025, only 41 percent of citizens reported satisfaction with access to quality health care, compared with an OECD average of 64 percent—a steep drop from an already lagging 53 percent in the 2023 survey.[26]
Doctors, too, have been caught in the crosshairs of a health care system that increasingly favors profit-oriented providers. Turkey is experiencing a marked brain drain of medical workers to Europe, as doctors leave behind meager paychecks, oversubscribed hospitals with difficult working conditions, and an alarming prevalence of workplace violence directed at health care personnel.[27] Among those who remain, many have shifted from working in public hospitals to the better-paying and less strained private sector.[28] According to TTB statistics, over 21,000 specialists have left public sector hospitals between 2012 and 2025, leaving clinics and hospital departments across many provinces without vital specialist care.[29] Now, 27 percent of health care workers—and over 30 percent of specialists—work in private hospitals that serve a small fraction of the Turkish population.[30] Even as physicians’ participation in the private sector has stabilized, specialty preferences among top medical graduates have continued to shift toward high-income, private sector fields—specifically, dermatology, radiology, and reconstructive or aesthetic surgery.[31] As more doctors pursue specialties primed for medical tourism markets in travel hubs, public sector hospitals in underserved areas will continue to weaken.
The notion that the health care system has left ordinary citizens behind has become increasingly prevalent. One early rumbling of this perception emerged with rising anti-refugee sentiment in the late 2010s, when rumors that Syrian refugees were being prioritized in public hospitals became endemic in Turkish society.[32] The sense of being sidelined within the health care system has persisted and intensified with the growth of medical tourism,[33] leading former Health Minister Fahrettin Koca to publicly deny social media claims that foreign nationals receive preferential treatment in Turkey’s hospitals.[34] But even in the absence of formalized preferences for foreigners, the creation of bifurcated intake through foreign patient offices risks the de facto prioritization of international patients paying higher prices—a troubling global trend recently exposed in the United States organ transplant industry as well.[35] Opposition politicians have increasingly seized on this sentiment. In press briefings and parliamentary hearings, representatives from multiple parties have linked medical tourism, appointment shortages with public providers, and poor health outcomes, arguing that state policy prioritizes profit-driven providers even as ordinary citizens struggle to access basic care.[36]
Another reason that Turkish citizens feel left behind is that the care marketed as “low-cost” to patients flush with foreign currency has become unaffordable to them. Turkey’s current economic crisis, which started with a decline in the Turkish lira’s value in 2018 followed by a steep plummet in late 2021, has led to rampant and persistent inflation. For Turkish citizens, both rising SGK premiums and private health care services are becoming increasingly unaffordable as citizens grapple with the cost-of-living crisis. Moreover, weak regulation of price caps on services has led hospitals to further inflate service prices, well beyond the state-prescribed SGK reimbursement levels. [37] Even the middle class, which once could circumvent public service wait times by opting for private care, can no longer afford hospital fees, thereby stretching public facilities even further.[38]
Public facilities have responded by monetizing some same-day after-hours services for those willing to pay.[39] As domestic financial strain has made health care a luxury good, private hospitals have been further incentivized to prioritize profitable specialties sought out by foreigners.[40] One international patient coordinator explained to me that in their hospital, though only 10 percent of patients are foreign, “all our profits come from foreign patients . . . 70 percent of revenue, all the profit.”[41]
The marketization that underpinned the HTP now operates through the export logic of state-managed medical tourism, thereby deepening divides between those who can pay and those who cannot. What began as a project to extend health care to all citizens has evolved into a system that extends it to the world while making access at home increasingly unequal. As Dr. Güray Kılıç of the Private Practice Physicians’ Branch of the TTB summarized in a December 2025 panel: “Medical tourism normalizes the idea that those with greater financial means are entitled to better and more advanced healthcare, rendering it acceptable to treat health not as a right, but as a consumer good.”[42]
The Limits of Exporting Health Care
Turkey’s continued growth as a medical tourism destination is neither inevitable nor costless. The sector’s rise has been enabled by reforms that tied health care expansion to market incentives—but this move also renders the industry vulnerable. The country’s capricious economy, changing global health care inequalities, and plateauing foreign demand have all exposed the fragilities of a health care system pursuing growth through foreign currency rather than prioritizing domestic need.
The cosmetic sector reveals both the potential boon and burden of a foreigner-facing health care model. Social media platforms are saturated with patient testimonials touting age- and gravity-defying physical transformations that reinforce Turkey’s reputation as an affordable aesthetic hub. But the same platforms that propel the industry can also undermine it. Stories of botched procedures go viral swiftly, imperiling the country’s international health care sector as isolated horror stories come to dominate social media.[43] The government has put forth policies to regulate the medical tourism market so as to stabilize a narrative of high quality and low prices. These efforts, then, must confront the uncomfortable reality that the informal market poised for greater regulation also drives down the prices that draw many patients from abroad.
At the same time, medical tourism is shifting from a technocratic growth strategy to an arena of domestic political controversy. The export orientation of health care has generated resistance among professional associations and sharpened opposition critiques of privatization at the expense of public care. As dissatisfaction with access has grown and health outcome gains have stalled, medical tourism has become a symbol of the relegation of Turkish citizens within a health care system that privileges an individual’s market position over their national membership.
A premier export has become an embattled public good for citizens, leaving them frustrated with an industry that was once touted as way to improve economic vitality and health care quality for all. So long as global celebrities and influencers continue to travel to Istanbul to renew their hairlines and Hollywood smiles, Turkey’s most visible export will continue to be its capacity to sell the promise of personal transformation to outsiders—all while collective care at home gradually frays. If access to care increasingly favors purchasing power over citizenship, the consequences may extend beyond hospital corridors. Universal health care was once a cornerstone of the AKP’s social contract—and its perceived reversal in pursuit of export-led growth risks reinforcing mounting doubts about the party’s capacity to deliver material improvements in citizens’ lives.
Nihal Kayali is a junior research fellow at the Crown Center and incoming assistant professor of sociology at Brandeis University.
For more Crown publications on topics covered in this Middle East Brief, see “After the Earthquake: The Politics of Disaster Response in Turkey,” “Beyond Erdoğan: Lessons from Turkey's 2024 Local Elections,” and “Turkey’s Economic Crisis and Erdoğan’s Multiple Rapprochement Initiatives.”
[1] Ceylan Yeginsu, “Why Medical Tourism Is Drawing Patients, Even in a Pandemic,” New York Times, January 19, 2021.
[2] Yeşim Sert Karaaslan, “Turkey to Open Doors to 31 Countries for Health Tourism,” Anadolu Ajansı, May 16, 2020.
[3] Alex Abad-Santos, “What It Means When Someone Says ‘He Went To Turkey’” Vox, December 18, 2024.
[4] Volkan Yılmaz, The Politics of Healthcare Reform in Turkey (Cham, Switzerland: Springer International Publishing, 2017).
[5] Tuba İ. Ağartan, “Marketization and Universalism: Crafting the Right Balance in the Turkish Healthcare System,” Current Sociology 60, no. 4 (June 2012): 456–71.
[6] Onur Hamzaoğlu, “Turkey’s Social Security System, Private Hospitals and the Function of the World Bank,” Bianet, April 23, 2025.
[7] Volkan Yılmaz and Püren Aktaş have published a deeply researched article that spells out in far greater detail many of the dynamics I describe in this Brief about the state’s role in steering medical tourism in the aftermath of state healthcare reforms. See “The Making of a Global Medical Tourism Destination: From State-Supported Privatisation to State Entrepreneurialism in Healthcare in Turkey,” Global Social Policy 21, Issue 2 (December 23, 2020): 301–18.
[8] Kayıhan Pala, Özgür Erbaş, Eriş Bilaloğlu, Bayazıt İlhan, Raşit Tükel, and Sinan Adıyaman. 2018. “Public-Private Partnership in Health Care: Case of Turkey,” World Medical Journal 64(4) (October 2018): 44–48.
[9] “Bakan Koca, Şehir hastaneleri, Türkiye’yi sağlık turizminde önemli bir marka haline getirecek [City hospitals will make Turkey a significant brand in health tourism],” Independent Türkçe, May 21, 2020.
[10] “Fahrettin Koca 6 yıllık bakanlığında 12 hastane yaptı: 12 hastanenin tümü teşvikli ve kamu arazileri üzerine yapıldı [Fahrettin Koca built 12 hospitals during his 6-year tenure as minister: all 12 hospitals were subsidized and constructed on public land],” Cumhuriyet, May 9, 2025.
[11] Cumhuriyet Halk Partisi (CHP), Haftalık Bilgilendirme Raporu [Weekly Briefing Report], Week of August 28–September 3, 2023.
[12] Ayakta Teşhis ve Tedavi Yapılan Özel Sağlık Kuruluşları Hakkında Yönetmelik, Official Gazette No. 26788, February 15, 2008.
[13] World Bank Group, “Turkish Health Transformation Program and Beyond” (Results Briefs, April 2, 2018).
[14] Ali Ergur, Cansu Saral, Buse Akkaya, and Ceren Tunay, “Yüze Kozmetik Müdahale Pratik Alanında Tıp-Piyasa-Siyaset İlişkiselliği [The medicine-market-politics relationality in the field of practice of facial cosmetic intervention],” Anadolu Üniversitesi Sosyal Bilimler Dergisi 24, no. 4 (December 23, 2024): 1453–74.
[15] Ergin Hava, “Turkey’s Medical Tourism Sector Can Be a Hair-Raising Experience,” The National, October 1, 2016.
[16] Ministry of Health, Regulation on Hair Transplantation Units, May 6, 2023.
[17] Furkan Gencoğlu, “Around 1M People Came to Türkiye for Hair Transplant Last Year,” Anadolu Ajansı, January 11, 2023.
[18] “Türkiye Targets $20 Billion in Health Tourism Revenue by 2028,” Daily Sabah, January 19, 2025.
[19] Yılmaz and Aktaş, “The Making of a Global Medical Tourism Destination.”
[20] Republic of Türkiye, Ministry of Trade, “Heal in Türkiye.”
[21] “Uluslararası Sağlık Turizmi ve Turistin Sağlığı Hakkında Yönetmelik,” Official Gazette No. 32882, April 26, 2025.
[22] “TTB’nin, İptali Talebiyle Dava Açtığı Uluslararası Sağlık Turizmi ve Turistin Sağlığı Hakkında Yönetmelik’e İlişkin Hukuki Bilgi Notu,” Türk Tabipleri Birliği (TTB) (Turkish Medical Association), July 18, 2025.
[23] Damla Polat, “Hekimler Kadiköy’den seslendi: ‘Mesleki bağımsızlık ve serbest calışma hakkımız engelleniyor,’” Cumhuriyet, February 22, 2026.
[24] Merve Safa Akıntürk, “29 kamu hastanesi sağlık turizmine açılıyor [29 public hospitals open to health tourism],” Yeni Şafak, July 4, 2025.
[25] Osman Öztürk, “Özel hastaneler pastanın kremasını sıyırıyor [Private hospitals skim the cream off the cake],” BirGün, October 13, 2025.
[26] “OECD Health at a Glance 2025: Türkiye,” November 13, 2025, and “OECD Health at a Glance 2023 Country Note: Türkiye.”
[27] Carlotta Gall, “Turkey’s Doctors Are Leaving, the Latest Casualty of Spiraling Inflation,” New York Times, February 7, 2022.
[28] Yusuf Tuna Koç, “Dr. Osman Öztürk: The Government Is Destroying Public Health for the Sake of the Private Sector,” BirGün, August 18, 2025.
[29] Sibel Bahçetepe, “Bir stadyum dolusu hekim istifa etti [A stadium full of doctors has resigned],” BirGün, December 3, 2025.
[30] T.C. Ministry of Health, “Sağlık İstatistikleri Yıllığı 2024 Haber Bülteni [Health Statistics Yearbook 2024 Press Release],” September 30, 2025.
[31] Dilara Bakan Kalaycıoğlu, “1987’den 2017’ye Hekimlerin Uzmanlık Alanı Tercih Değişimleri [Changes in Physicians’ Speciality Preferences from 1987 to 2017],” Tıp Eğitimi Dünyası 19,59 (2020): 158–71;“Eylül 2023 TUS Yerleştirmeleri ile İlgili Bilgi Notu [Information Note on Medical Specialty Exam (TUS) Placements,” Ankara Tabip Odası (ATO), 12 September 12, 2023.
[32] Selin Siviş, “Who Is (Un)deserving? Differential Healthcare Access and the Interplay between Social and Symbolic Boundary-Drawing towards Syrian Refugees in Turkey,” Journal of Ethnic and Migration Studies 48, no. 17 (April 6, 2022):4029–48.
[33] Ceren Deniz, “Antalya’da yabancı hasta sezonu: ‘Doktorumuz artık yerli hastalara bakmıyor’” [Foreign patient season in Antalya: “Our doctor no longer cares for local patients],” Gazete Duvar, July 2, 2023.
[34] Burcu Çalık Göçümlü, “Bakan Koca’dan ‘yabancı uyruklu kişilerin “öncelikli hasta” muamelesi gördüğü’ iddialarına yanıt [Minister Koca's response to allegations that “foreign nationals are treated as 'priorly patients’”],” Anadolu Ajansı, June 24, 2023.
[35] Brian M. Rosenthal and Mark Hansen, “Hospitals Cater to ‘Transplant Tourists’ as U.S. Patients Wait for Organs,” New York Times, December 16, 2025.
[36] Weekly CHP briefing, Week of August 28–September 3, 2023. See also CHP representative Kayıhan Pala’s remarks in TBMM, 28th Term, 4th Legislative Year, 31st Sitting – General Assembly Transcript. Parliamentary Proceedings, 2025.
[37] Koç, “Dr. Osman Öztürk: The Government Is Destroying Public Health.”
[38] Damla Polat, “Devlet hastanelerinde randevu bulamayan hastalar artık özel hastaneye de gidemiyor: Parası olan yaşayacak [Patients who cannot find appointments at public hospitals can no longer go to private hospitals either: Those who have money will survive],” Cumhuriyet, November 6, 2024.
[39] Sibel Bahçetepe, “Hem kamuda hem özelde hastadan ek ücret isteniyor: Ayni güne MR ama parası olana [Additional fees are demanded from patients in both public and private sectors: Same-day MRI, but only for those who have money],” BirGün, October 20, 2025.
[40] Nefes Pirzada, “The Expansion of Turkey’s Medical Tourism Industry,” Voices in Bioethics (June 15, 2022).
[41] Interview with international patient coordinator, July 2025.
[42] “‘Hizmet Ticareti, Sağlık Turizmi ve Mesleğe Etkileri’ Paneli Yapıldı [Panel held on ‘Trade in Services, Health Tourism, and Effects on the Profession’],” Türk Tabipleri Birliği, December 29, 2025.
[43] Aida Fofana, “‘I paid £6k to Feel Worse Than I Did before Surgery,’” BBC News, December 4, 2024, and Juliana Cruz Lima, “OP Horror: Brit Tourist, 38, Dies after Turkey Hair Transplant Goes Wrong with Probe Launched into Clinic,” The Sun, July 31, 2025.
Recommended Citation: Kayali, Nihal. “Medical Tourism and Public Health Care in Turkey” Middle East Brief, no. 168. Crown Center for Middle East Studies, Brandeis University, April 2026.
The opinions and findings expressed in this Brief belong to the authors exclusively and do not reflect those of the Crown Center or Brandeis University.